ANTIETAM BATTLEFIELD WALK
The Antietam Battlefield Staff Walk is an important professional activity that combines historical lessons from a pivotal battle; analysis of strategic, operational, and tactical decision-making; and how military medical practice and leadership supports warfighter missions and objectives.
Following an introductory battle analysis, this USU learning activity reinforces student knowledge of the six principles of health service support: conformity, proximity, flexibility, mobility, continuity, and control. At various points around the battlefield, faculty and students discuss examples of the principles in action. A reflective activity afterwards asks participants to share their observations and insights as they might apply to the battlefields of the present and future.
MEDICAL FIELD PRACTICUMS
Students participate in a Medical Field Practicum (MFP) during each of their four years at USU. These experiences are structured appropriately for the level of accumulated medical knowledge in the School of Medicine curriculum. They then add new military-unique skills and practical applications that build upon one another. Clinical abilities in military field medicine are developed from basic self-aid and buddy care using the concepts developed in Tactical Combat Casualty Care (TCCC) to primary responsibility for simulated combat casualties in a notional Role-1 setting. Knowledge in military medical practice transitions from preparing for small-team responses to planning joint health services at the tactical and operational levels. Working environments become more and more extreme, and ethical and legal decision making become increasingly challenging. The focus of military medical leadership expands from personal to interpersonal to team to organizational levels. For more information and dates for upcoming medical field practicums, please see the document link below.
MEDICAL FIELD PRACTICUM 101
MFP 101 is conducted after the first didactic module in the first year of medical school. Content includes didactic and practical experiences that supplement Service-specific officer schools with regard to skills needed to survive and operate in deployed settings, the basics of joint health services and casualty evacuation in contingency operations, experiencing what it is like to be a patient in a simulated environment, and having discussions with senior non-medical military leaders regarding their perspectives on leadership and the roles, responsibilities, and interfaces of medical officers.
Upcoming Military Field Practicum Dates
MEDICAL FIELD PRACTICUM 102 “ACME”
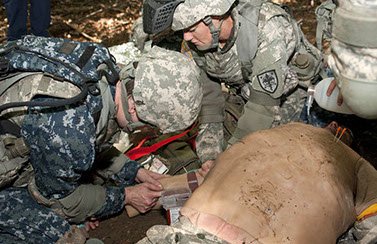
MFP 102 is also called the Advanced Combat Medical Experience (ACME) and consists of didactic and practical components aimed at expanding Forward Resuscitative Care (FRC) skills. It is conducted at the beginning of the second year of medical school and builds on skills learned in Combat Medical Skills (CMS) during the latter half of the first year.
The didactic component is comprised of a Tactical Combat Casualty Care (TCCC) refresher course with skills practice and demonstration, an introduction to battlefield pain management, and discussions with a panel of Wounded Warriors.
Practical exercises focus on delivering lifesaving care for one or two simulated combat casualties in a field setting using TCCC concepts and procedural skills. Leadership abilities are evaluated at the level of teams of 2–5 individuals and focus on crisis communications while stressed.
Military and Emergency Medicine Department Upcoming Field Practicum Dates
MEDICAL FIELD PRACTICUM 201 “OPERATION GUNPOWDER”
MFP 201 is a prolonged casualty care field exercise for third year medical students in the Uniformed Services University School of Medicine and Graduate School of Nursing. The 36 hour simulated, austere combat environment allows students to participate in all aspects of patient care. Students work together in squads exercising medical and military roles to complete their mission.
The course places post-clerkship students into leadership positions in teams of 6-8 individuals in order to demonstrate competency in performing Tactical Field Care, Forward Resuscitative Care, Prolonged Field Care, Casualty Evacuation, integrating with Forward Resuscitative Surgery teams, Medical Evacuation, and preparing patients for Critical Care Air Transport during simulated operations in a physically isolated and medically austere environment. Students are also exposed to concepts and principles of Forward Resuscitative Surgery and Critical Care Aeromedical Transport.
Faculty members consist of medics, nurses, and physicians with significant personal experiences in deployed settings. The special-operations communities of all Services provide significant support for MFP 201.
MEDICAL FIELD PRACTICUM 202 “OPERATION BUSHMASTER”
The Military Contingency Medicine (MCM) Course and MFP 202 combine to ensure USU graduates enter internship and subsequent assignments to operational units with the finely honed skills, experience, and character they will need to take on the ever-changing challenges facing our armed service members across the globe.
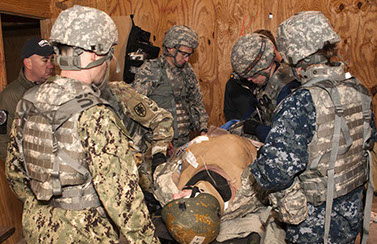
The MCM Course is a two week course which takes place at the Uniformed Services University. Students receive lectures on topics related to deployment medicine and practice critical hands on Tactical Combat Medicine skills. MFP 202 is conducted at Fort Indiantown Gap, Pennsylvania, midway through the 15 months when students attend advanced clinical clerkships. Operation Bushmaster allows medical students—along with students from USU Graduate School of Nursing and international medical students and physicians—to test their knowledge, skills, and abilities in military field medicine, military medical practice, and military medical leadership in a simulated, resource constrained, far-forward tactical field setting similar to a Role-1 capability during a contingency deployment. One day is set aside for planning and rehearsals prior to four days of intense operations.
Mission sets include combat and stability operations. Students rotate through various roles ranging from medic to unit healthcare provider to the leader of a unit with 20–25 individuals. These teams are presented with simulated illnesses, injuries, and operational problems that reflect broad types of challenges across many domains: integration with the commanders plans, military planning processes, combat casualty care, triage skills and mass-casualty management, return-to-duty versus evacuation decisions, employment of telemedicine, knowledge of the Law of Armed Conflict, stress management, ethical dilemmas, working with other cultures and communicating through interpreters, interacting with the media, and many more.
Dozens of faculty members formally assess and evaluate leadership skills and healthcare-delivery skills. Evaluation teams are composed of local and national USU faculty, subject-matter experts, and civilian volunteers from around the globe.
Upcoming Field Practicum Dates